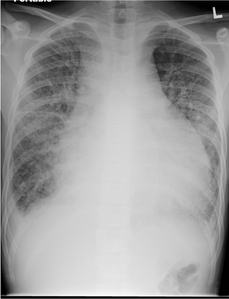
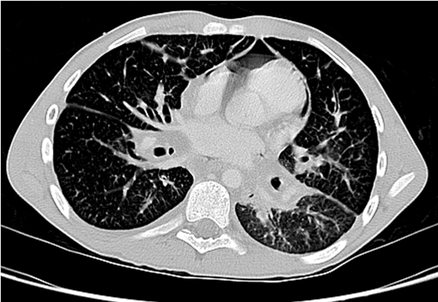
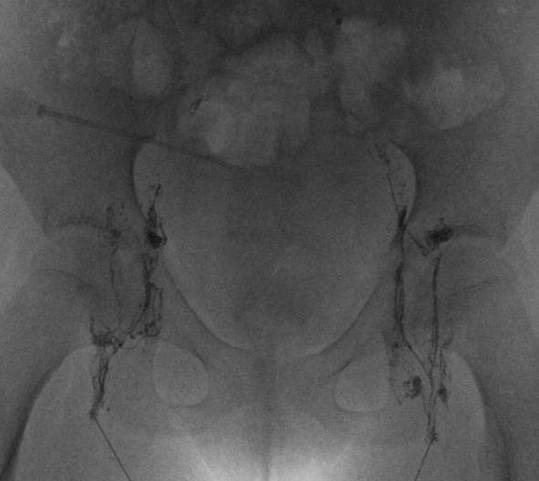
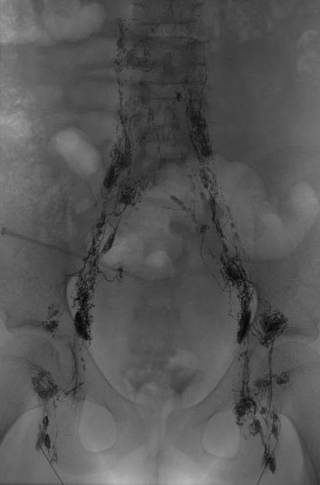
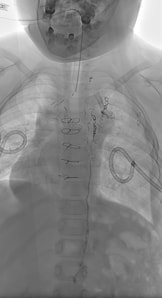
Intranodal Lymphangiography
Indications |
|
Contraindication |
|
Pre-procedure |
|
Technique |
Supplies
Prep
Technique
|
Complications |
|
|
|
|
Thoracic Duct Embolization
Technique |
|
Complications |
|
References |
|